ल्व्हंल्वय्
| ल्व्हंल्वय् (Obesity) वर्गीकरण व पिनेया स्रोत | ||
 | ||
|---|---|---|
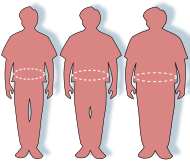
| साधारन, ल्व्हंगु व ल्व्हंल्वय् क्यनातःगु किचःकिपा व जंया परिधिकिपा | ||
| ICD-10 | E66. | |
| ICD-9 | 278 | |
| OMIM | 601665 | |
| DiseasesDB | 9099 | |
| MedlinePlus | 007297 | |
| eMedicine | med/1653 | |
| MeSH | C23.888.144.699.500 | |
ल्व्हंल्वय् (Obesity) म्हया दा तस्कं अप्वया उसाँय् मभिनिगु, मनुया आयु म्हो जुइगु व/वा ल्वचं कइगु (उसाँय्या समस्या वइगु) छता चिकित्सा शास्त्रया अवस्था ख। [१][२] मनुया बदि मास इन्देक्स (BMI)[३] छ्यला मनुयात ल्व्हंल्वचं काःगु दु-मदूगु स्वयेगु याइ। बदि मास इन्देक्स धाःगु मनुया तौलयात धिकःया स्क्वायरं दिभाइद याना वःगु छगू रेसियो ख। थ्व रेसियो ३०kg/m2 स्वया अप्व दःसा मनुयात ओबिस धाइ।
ल्व्हंल्वचं काःगु मनुतयेत नुगःया ल्वय्, ताइप २ दायबितिज, अब्स्त्रक्तिभ स्लिप अप्निया, छुं क्यान्सर, व अस्तियोआर्थ्राइतिस आदि थें न्यागु थी-थी ल्वचं कायेगु व थ्व ल्वय्त तच्वःया सीगु सम्भावना अप्व दु। [२] ल्व्हंल्वय्या दकलय् साधारन कारणय् अप्व नयेगु, म्हो शारीरिक व्यायाम यायेगु, वंशानुगत सम्भावना आदि मू कारण ख। छुं अवस्थाय् धाःसा जीन, इन्दोक्राइन व्याधि, वासः वा मानसिक ल्वचं नं ल्व्हंल्वय् जुइफु। म्हो जक्क नःसां पाचन बिस्तारं जुया ल्व्हनिगु धैगु विचाः समर्थन यायेगु दसिं मगा। साधारणकथं ल्व्हंपिं मनुतयेत इमिगु अप्वःगु बदि मास इन्देक्सया कारणं म्ह्वय् अप्व उर्जा मा।[४][५]
ल्व्हंल्वय्या मू निदान अप्सं च्वनिगु व शारीरिक व्यायाम ख। अप्व उर्जा दूगु नसाः दसु दा व चिनि म्हो जक्क नया दायतरी फाइबर अप्व दूगु नसाः नया थ्व ल्वय् नियन्त्रण यायेछिं। ल्व्हंल्वय् विरोधी वासःत नं विकशित जूगु दु। थन्यागु वासलं मनुयात नेप मत्यायेगु व दाया स्वसन म्हो याइ। नसाः, व्यायाम व वासलं ल्व्हंल्वय्यात मथ्युसा ग्यास्त्रिक बलुन वा बेरियात्रिक सर्जरी छ्यला प्वाया आयतन म्हो यायेगु वा आन्द्राया हाकः चिहाकेगु याना मनुयात याकनं हे प्वा जायेकिगु वा नसांः म्हो जक्क पोषक तत्त्व स्वसन यायेगु अवस्था दयेकेछिं। [६][७]
हलिमय् हे ल्व्हंल्वय् मनु मदइगु छगू पनेछिंगु कारणय् मू कारण ख। थ्व ल्वचं कापिं ल्वमितेगु (तःधंपिं व मस्त) ल्या अप्वया वैच्वंगु दु। उसाँय् थुवातेसं थ्व ल्वय्यात २११गु शदीया दकलय् च्युता यायेमाःगु सार्वजनिक उसाँय्य् छगूया रुपय् कयाच्वंगु दु। [८] सामाजिक कथं, न्हापा न्हापा कूलीनता, वैभव व प्रजननशीलताया चिंया रुपय् कयातःगु ल्व्हनिगु अवस्था आधुनिक हलिमय् वया लांछनीय व मभिंगु चिंया रुपय् खनावःगु दु। [२][९] सन् २०१३स अमेरिकन मेदिकल एसोसियसनं तच्वःकं ल्व्हंगु अवस्थायात ल्वय्या रुपय् परिभाषित याःगु दु। [१०][११]
लिधंसा
[सम्पादन]- ↑ WHO 2000 p.6
- ↑ २.० २.१ २.२ Cite error: Invalid
<ref>tag; no text was provided for refs namedHaslamJames - ↑ WHO 2000 p.9
- ↑ Kushner, Robert (2007). Treatment of the Obese Patient (Contemporary Endocrinology). Totowa, NJ: Humana Press. Retrieved on April 5, 2009.
- ↑ Adams, PG (July 2000). "Obesity in anaesthesia and intensive care". Br J Anaesth 85 (1): 91–108. DOI:10.1093/bja/85.1.91. PMID 10927998.
- ↑ NICE 2006 p.10–11
- ↑ Imaz, I (July 2008). "Safety and effectiveness of the intragastric balloon for obesity. A meta-analysis". Obes Surg 18 (7): 841–6. DOI:10.1007/s11695-007-9331-8. PMID 18459025.
- ↑ Barness, LA (December 2007). "Obesity: genetic, molecular, and environmental aspects". American Journal of Medical Genetics 143A (24): 3016–34. DOI:10.1002/ajmg.a.32035. PMID 18000969.
- ↑ Cite error: Invalid
<ref>tag; no text was provided for refs namedWoodhouse - ↑ Pollack, Andrew. "A.M.A. Recognizes Obesity as a Disease", June 18, 2013.
- ↑ The Facts About Obesity. American Hospital Association (June 21, 2013). June 24, 2013 कथं।
| विकिमिडिया मंका य् थ्व विषय नाप स्वापु दुगु मिडिया दु: Obesity |
